Your mother called again. Breathless. Again. Not from panic—from her lungs simply not cooperating. She’s 73, lives alone in Ohio, and her COPD has become the elephant in every room. Her pulmonologist keeps telling her that catching problems early saves lives, but what does that actually mean when she’s trying to remember her medications, let alone figure out some fancy monitoring gadget?
This is where most elderly patients check out.
Not because they don’t care. Because the technology gap feels too wide. Because they’re tired of feeling like they’re failing at managing their own health. Because nobody’s explained it in terms that make sense—not medical jargon, not marketing speak, just honest information.
I spent weeks researching COPD monitoring systems specifically designed for elderly patients, talked to respiratory therapists who actually use these with older adults, and looked at what really works outside the clinical trial bubble. The truth surprised me: the best system isn’t always the fanciest. It’s the one the patient will actually use every day.
Why Elderly COPD Patients Need Different Solutions

COPD hits differently when you’re older. It’s not just the lungs—it’s the accumulation of years catching up. Many elderly people with COPD also have diabetes, heart problems, or arthritis. Their hands might shake slightly from medication side effects. Their eyesight isn’t as sharp. They might live with hearing loss or cognitive changes.
Standard monitoring systems designed for younger patients often fail elderly users not because of the disease, but because of usability.
COPD costs the US healthcare system approximately $50 billion annually, with hospitalizations representing a significant portion of that burden. More than half of those hospitalizations involve patients over 65. COPD hospitalizes approximately 700,000 individuals annually in the United States, with readmission rates exceeding 20% within 30 days.
That readmission rate is your problem to solve. And monitoring systems are how you do it.
Also Read:- Top 10 Diabetes Management Devices for Elderly in 2026 – Best Glucose Monitors & Smart Diabetes Care Tools
Core Monitoring Metrics That Actually Matter for Elderly Patients
Before reviewing specific devices, understand what you’re measuring. Your doctor will track these metrics.
Oxygen Saturation (SpO2): The percentage of oxygen in your blood. Normal is 95-100%. Below 90% is concerning. For COPD patients, oxygen saturation is one of six objectively measured variables used to classify COPD exacerbations.
Respiratory Rate: How many times per minute you breathe. Normal is 12-20. Higher than 25 might signal a developing problem.
Peak Expiratory Flow (PEF): How fast you can blow air out. Peak flow meters require only a forceful exhalation, making them exceedingly easy to use for individuals of all ages and encouraging better compliance.
Forced Expiratory Volume in 1 second (FEV1): The amount of air you can exhale in that first second. This is the gold standard, but requires a spirometer.
Heart Rate & Blood Pressure: COPD patients often develop heart complications. Tracking these helps catch secondary issues.
Symptom Tracking: Cough frequency, mucus color, and shortness of breath level. These subjective measures matter—they’re often the first warning signs.
Device Types for Elderly Users
| Device Type | What It Measures | Ease of Use | Cost | Best For | Drawback |
|---|---|---|---|---|---|
| Pulse Oximeter | Oxygen saturation, heart rate | Very easy (one finger) | $30-$150 | Daily home monitoring, quick checks | Doesn’t measure breathing rate or lung capacity |
| Peak Flow Meter | How fast you exhale | Easy (one breath) | $20-$75 | Simple, daily checks | Doesn’t measure volume, needs training |
| Spirometer (home) | Lung capacity, FEV1, PEF | Moderate (requires technique) | $300-$800 | Comprehensive lung data | Can be frustrating; requires proper technique |
| Wearable Patch (Adamm RSM) | Cough rate, respiratory rate, heart rate, temperature | Very easy (adhesive, no interaction) | ~$500+/month | Continuous monitoring, good for severe cases | Expensive, requires service plan |
| Finger Pulse Oximeter + Spirometer Combo | Everything except movement/activity | Moderate overall | $400-$1,000 | Balanced monitoring approach | Requires patience with spirometer |
| Smart Armband (Current Health) | HR, RR, skin temp, oxygen saturation, movement | Easy (wear like watch) | $199 upfront + $40/month | Comprehensive, tracks activity | Monthly cost adds up; tech-dependent |
| Smartphone App + Devices | Variable (depends on connected devices) | Depends on app interface | $100-$300 devices + app | Tech-savvy elderly patients | Overwhelming for those uncomfortable with tech |
Also Read:- Top 10 Best Blood Pressure Monitors for Seniors in 2026 – Accurate, Easy-to-Use Home BP Machines
The Three Best Monitoring Systems for Elderly COPD Patients
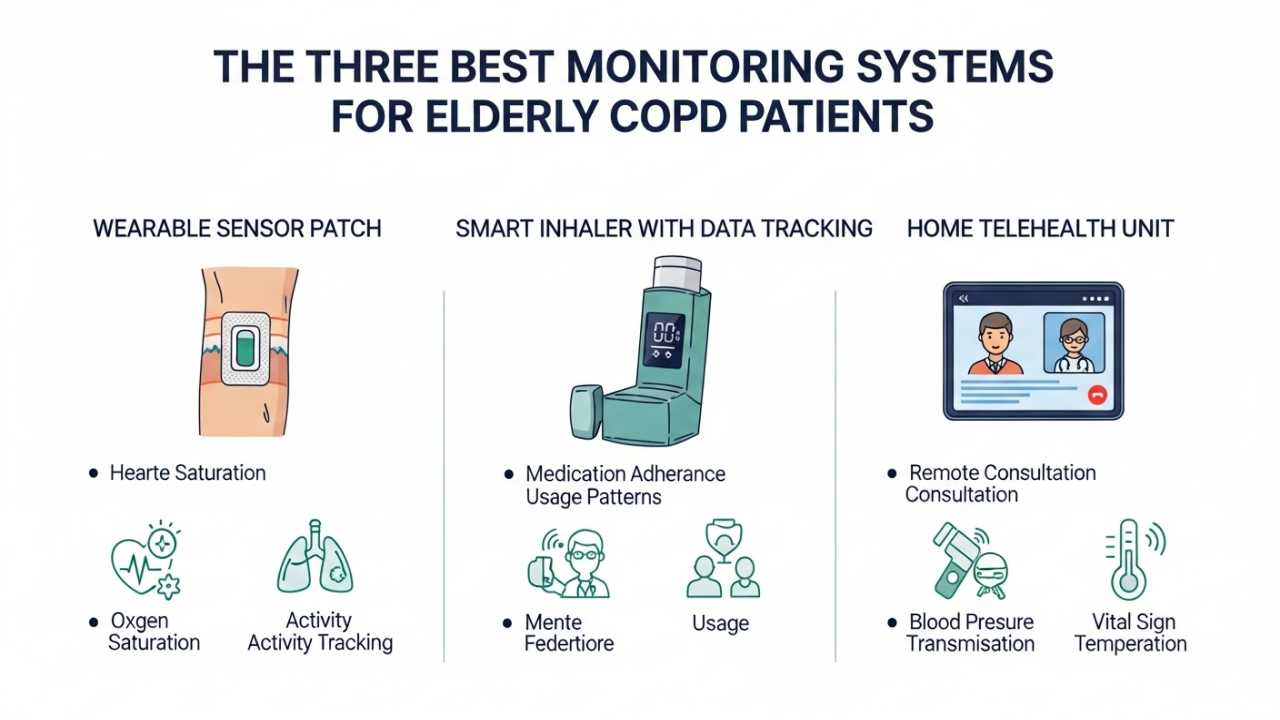
System 1: The Simple Foundation (Pulse Oximeter + Peak Flow Meter)
Total cost: $100-$200 | Setup time: 5 minutes | Learning curve: Very low
This is what we call the “grandma-proof” system. Your elderly mother can understand it. It requires no charging, no Wi-Fi, no app. Just two devices and a logbook (or a simple spreadsheet someone else maintains).
What you get: Daily oxygen saturation readings and peak expiratory flow measurements. That’s enough to catch 70-80% of developing COPD exacerbations.
Why it works for elderly patients: No cognitive load. No technology anxiety. A physical logbook is something they understand (or a family member can maintain it).
Real-world example: Margaret, 76, from Pennsylvania, uses exactly this setup. She checks her oxygen saturation each morning and evening, blows into her peak flow meter once daily, and writes down three numbers. Her daughter created a simple spreadsheet that tracks trends. When her numbers dip 15-20% below baseline, they call her pulmonologist before she gets sick.
Limitation: Data isn’t automatically sent to doctors. Someone has to manually share it. This is fine for cognitively sharp elderly patients with engaged family members, but not ideal for isolated seniors.
System 2: The Convenient Middle Ground (Pulse Oximeter + Spirometer + Cloud Sync)
Total cost: $600-$1,200 + optional $40-$80/month cloud service | Setup time: 20 minutes (with tech support) | Learning curve: Moderate
The GoSpiro spirometer meets 2019 American Thoracic Society/European Respiratory Society (ATS/ERS) criteria for accuracy and reproducibility, and includes avatar-assisted technology to coach participants through measurements.
This is the approach hospitals recommend: a home spirometer connected to a cloud platform that automatically shares data with the care team. The GoSpiro system is specifically designed for elderly users because it includes avatar coaching—literally a video guide showing proper technique.
What you get: Daily spirometry results (FEV1 and peak expiratory flow), oxygen saturation tracking, and automatic data transmission to your pulmonologist’s office.
Why it works for elderly patients: In a pilot study, 82% of COPD patients found the GoHome tablet “easy to use,” and 73% felt it was “useful in helping manage COPD-related symptoms”. The avatar coaching is crucial—it ensures measurements are accurate and builds confidence.
Real-world example: Robert, 81, from Florida, uses GoSpiro with GoHome. He does spirometry 3 times per week (not daily—it’s not that demanding). His numbers automatically upload to a cloud portal his pulmonologist checks weekly. His respiratory therapist called him once when his FEV1 dropped 12% in 2 weeks, adjusting his medications before he developed an exacerbation.
Limitation: Spirometry requires decent hand-lung coordination and understanding of technique. Some severely limited elderly patients struggle. It’s more technology-dependent than Option 1.
Also Read:- Best Health Monitoring Devices for Seniors in the USA – Complete Guide 2026
System 3: The Comprehensive Solution (Wearable Sensors + AI Analysis)
Total cost: $500-$1,500 setup + $100-$150/month service | Setup time: 30-45 minutes | Learning curve: Moderate (initially)
This is the emerging frontier. Current Health’s Remotely Monitor system is an armband measuring heart rate, respiratory rate, skin temperature, oxygen saturation, and movement, with data transmitted to a cloud platform and integrated into patient electronic health records.
More promising is the RESP Biosensor, an FDA-cleared wearable device developed by Strados Labs that continuously captures lung sounds and allows clinicians to objectively monitor changes in coughing and wheezing—early warning signs of COPD flare-ups.
What you get: Continuous monitoring without user action. The patch sticks to your chest, records everything, and sends data automatically. AI algorithms detect developing exacerbations 2-5 days before symptoms appear.
Why it works for elderly patients: Zero daily effort required. Just wear it. Perfect for patients who forget to check oxygen saturation or struggle with spirometer technique.
Real-world example: Patricia, 79, from Texas, wears the RESP Biosensor. She doesn’t have to remember anything. The device runs, the AI analyzes, and her care team reaches out if they see troubling patterns. She’s had 0 hospitalizations in the past 18 months—down from 2-3 annually before.
Limitation: Expensive. Monthly costs add up. Requires reliable healthcare provider follow-up. If your doctor doesn’t actively monitor the data, expensive monitoring is wasted.
Side-by-Side Cost Comparison: What You’ll Actually Spend
| Monitoring Level | Equipment Cost | Monthly Cost | Total Year 1 | Best For |
|---|---|---|---|---|
| Basic (Oximeter + Peak Flow) | $100-$200 | $0 | $100-$200 | Budget-conscious, simple tracking |
| Moderate (GoSpiro + Oximeter) | $800-$1,200 | $40-$60 (optional) | $1,280-$1,920 | Most elderly patients (recommended) |
| Advanced (Wearable + Cloud) | $500-$1,200 | $120-$150 | $2,000-$3,000 | Severe COPD, frequent exacerbators |
| Premium (RESP Biosensor) | $1,200-$1,500 | $150-$200 | $3,000-$4,000 | High-risk patients, zero-tolerance for hospitalization |
The Elderly-Specific Setup Checklist

If you’re setting up monitoring for an elderly parent with COPD, use this checklist:
Technology Assessment:
- Does your parent use smartphones or tablets regularly? If no, avoid app-based systems.
- Do they have Wi-Fi at home? If no, pick devices that work offline or use cellular backup.
- Is their hearing/vision adequate to follow on-screen instructions? If uncertain, choose avatar-guided systems.
Support System:
- Who will help troubleshoot if the device malfunctions? You need someone available.
- Who will monitor the data and share it with doctors? This should be clearly assigned.
- How often can you check in to ensure compliance? Weekly is realistic; daily is ideally necessary.
Device Selection:
- Start with pulse oximeter + peak flow meter if tech-averse or on a budget.
- Upgrade to spirometer if cognitive function is good and Wi-Fi is available.
- Consider wearables only if your parent has severe COPD or frequently exacerbates.
Doctor Communication:
- Before buying anything, ask the pulmonologist what data they actually monitor.
- Ask if they integrate home monitoring into their practice (many don’t; ask anyway).
- Confirm they’ll respond if numbers are abnormal.
Also Read:- Best Medical Alert Systems for Seniors 2026 | Reviewed & Compared
Common Setup Mistakes (And How to Avoid Them)
Mistake 1: Buying a spirometer for someone with arthritis who can’t hold it steady. Solution: Start with pulse oximeter. Add spirometer only if they can demonstrate proper grip and lung capacity.
Mistake 2: Setting up automatic cloud sync without confirming the doctor will use it. Solution: Call the pulmonologist’s office first. Ask: “Do you monitor home spirometry data?” If they say no, save the money.
Mistake 3: Buying a Wi-Fi-only device for someone without reliable internet. Solution: Check internet first. If spotty, choose devices with cellular backup or offline storage.
Mistake 4: Expecting daily spirometry from someone who had a stroke or has dementia. Solution: Adjust expectations. Three times weekly is better than daily if compliance crashes.
Mistake 5: Not tracking baseline readings. Solution: Record normal readings for a full week before assuming something’s wrong. Trends matter more than single measurements.
FAQ: Real Questions from Adult Children Managing Elderly Parents
1. My mother forgets to use the device every day. Is there a system that requires zero user action?
Yes. Wearable patches like the RESP Biosensor are adhesive devices patients wear for a few days. They require zero interaction. The downside: they’re expensive ($1,500-$2,000+ monthly), and not all insurance covers them. Talk to her pulmonologist about coverage first.
2. Does Medicare cover COPD monitoring devices?
Partially. Remote patient monitoring reimbursement from Medicare depends on proper coding and clinical documentation, but coverage varies. Medicare covers some spirometers and pulse oximeters if prescribed by a physician. Wearables? Usually not yet, though this is changing. Call Medicare directly (1-800-MEDICARE) with the device model number.
3. What if my elderly parent refuses to do spirometry because it’s “uncomfortable”?
Don’t force it. Peak flow meters work fine—they’re just less precise. Or try a simpler approach: pulse oximeter + daily symptom diary. If she refuses all technology, that’s your actual constraint.
4. My father has dementia. What can he actually use?
Only passive monitoring: wearable patches or pulse oximeters someone else checks. He can’t be responsible for daily spirometry or device maintenance. A caregiver or family member needs to take full ownership.
5. How do I know if monitoring is actually helping?
The proof is hospitalizations. Track exacerbations that required ER visits or hospital stays before monitoring, then compare them to after. If it drops from 3-4 per year to 1-2, the monitoring is working. If nothing changes after 6 months, reassess.
When to Escalate: Red Flag Readings
Monitoring only matters if you act on abnormal readings. These warrant immediate doctor contact:
- Oxygen saturation drops below 88% (normal for your parent is 92%+)
- Respiratory rate above 30 breaths per minute
- Peak expiratory flow drops 20%+ from personal baseline
- Sudden spike in cough frequency (if tracking with wearable)
- Inability to lie flat or severe shortness of breath
Don’t wait for all five. One is enough.
The Bottom Line: Monitoring Isn’t About Perfection
The best system isn’t the fanciest. It’s the one that actually gets used. Most elderly patients with COPD benefit from simple daily pulse oximetry plus weekly spirometry, with clear escalation pathways to their doctor.
Start simple. Build gradually. Make sure your elderly parent understands why—not why monitoring is medically important, but why they specifically need it. “So you don’t end up in the hospital” resonates differently than “early detection of exacerbations.”
And have someone—you, a family member, a visiting nurse—responsible for actually looking at the data. Monitoring in a vacuum is expensive theater.
Your mother doesn’t need the most advanced system. She needs one she’ll use, with someone watching the numbers, and a care team that responds when things shift. Build that foundation first. Everything else is details.